Kris T. Huang, MD, PhD, CTO
Have you ever wondered how far we’ve come in image registration technology? It wasn’t always the case that 3D deformable registration could be fully automated. This week, we’re throwing it back to 1895, when medical imaging started, then we’ll go back to the future to see how medical image registration evolved.
The discipline of radiology began with the first X-ray images taken by Wilhelm Röntgen in 1895, and the medical applications of non-destructively imaging the internals of the human body were immediately obvious. Perhaps equally obvious was the utility of establishing a clear spatial relationship (registration) between multiple images to facilitate comparisons, given the appearance of side-by-side plaques produced less than a year later.
Radiology’s digital roots, however, began with the introduction of 3D imaging into clinical practice with the first CT scan performed in 1971. Although that first image had a slice pixel resolution of only 80×80 (comparable to a modern desktop icon), by 1975 image resolution had increased to 320×320, and by 1978 scanners started to produce a more modern 512×512 image matrix. MRI entered the scene with its first clinically useful image in 19801. Ironically, it wasn’t until 1983 that 2D digital radiography entered clinical use2.
By 1980 about 3 million scans were performed annually in the United States, and by 2007, over 70 million CT studies were ordered and performed each year3. According to a report from EMC and the research firm IDC4, worldwide digital healthcare data is expected to reach 2.3 zettabytes (23×109 terabytes) by 2020, and 90-95% of that is radiologic data.
Extrapolating from the NHS Annual Imaging and Radio- diagnostics Data5, last released for 2014, 3D medical imaging conservatively accounts for about 20% of all radiodiagnostic examinations in the UK, and is likely higher for countries like the US6.
The nuclear medicine age
Although published research for simple alignment of low resolution brain scans dates back to the 1970s, the value of image (co-)registration as a prerequisite for extracting higher level data from images didn’t truly surface until the early 1990s, when nuclear medicine scans started to provide functional information, not just anatomic information.
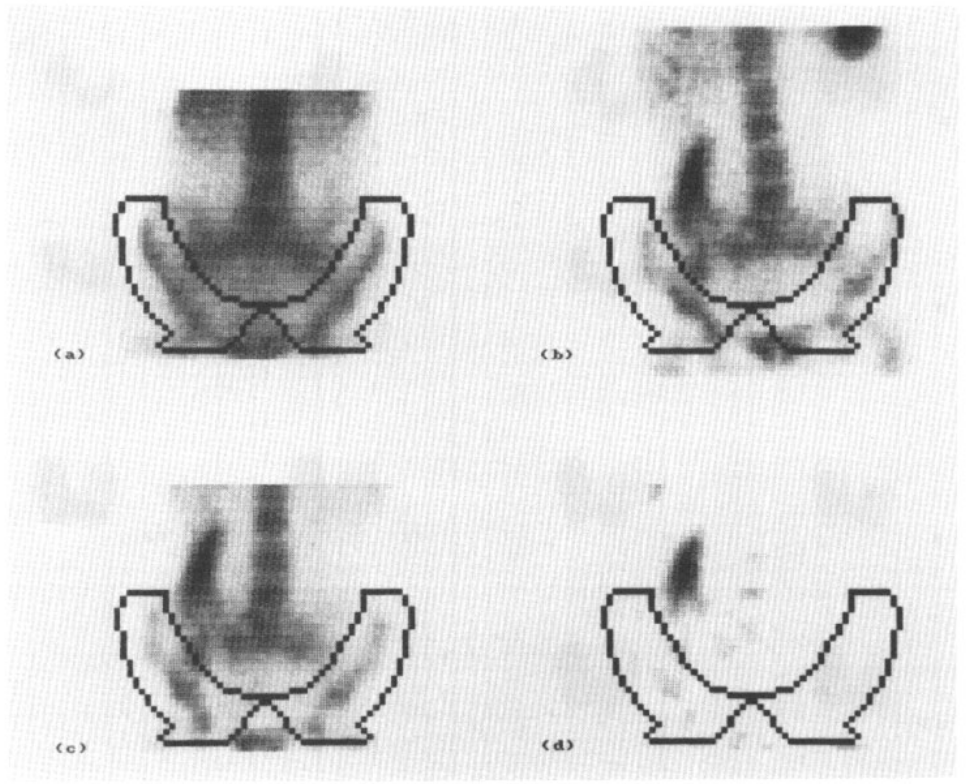
1991. Example of semi-automatic 2D registration of a tagged white blood cell scan from a patient with Crohn’s disease. Registration allows background subtraction of normal activity (top left) from the abnormal state (unregistered: top right; registered, bottom left) to highlight the flare region (bottom right). Registration focus outlined in black. Image from (7).
The introduction of 3D positron emission tomography (PET) in the early 1990s8 popularized a new idea, image fusion, and brought image registration into the third dimension. The functional information of PET could be combined, or fused, with the anatomic information of CT or MRI into a single, concise image.
Considering PET-CT is the most common combination today, it is somewhat surprising that the first research papers on automatic multimodality registration of PET data actually describe PET-MRI registration instead. At the time, MRI was preferred for its “intrinsically better resolution,”9 likely referring to its superior soft tissue definition. However, commercial combined PET-CT scanners beat availability of PET-MRI by about a decade, and the rest, as they say, is history.
 Example of a PET-CT image fusion combining anatomic data from a CT (top) with increased metabolic activity (middle) to highlight areas of active cancer (bottom). (Image credit: Wikipedia)
Example of a PET-CT image fusion combining anatomic data from a CT (top) with increased metabolic activity (middle) to highlight areas of active cancer (bottom). (Image credit: Wikipedia)
Next time, we’ll dig into the algorithms (no math, I promise!).
References
- http://www.bshr.org.uk/mallard.html
- Sonoda, M., Takano, M., Miyahara, J. & Kato, H. Computed radiography utilizing scanning laser stimulated luminescence. Radiology 148, 833–838 (1983).
- Brenner, D. J. & Hall, E. J. Computed Tomography — An Increasing Source of Radiation Exposure. New England Journal of Medicine 357, 2277–2284 (2007).
- https://www.emc.com/analyst-report/digital-universe-healthcare-vertical-report-ar.pdf
- https://www.england.nhs.uk/statistics/statistical-work-areas/diagnostics-waiting-times-and-activity/imaging-and-radiodiagnostics-annual-data/
- http://chapter.aapm.org/NE/DOCUMENTS/20021010.pdf
- Barber, D. C. Registration of low resolution medical images. Physics in Medicine and Biology 37, 1485–1498 (1992).
- Wagner, H. N. Clinical PET: its time has come. J. Nucl. Med. 32, 561–564 (1991).
- Woods, R. P., Mazziotta, J. C. & Cherry, S. R. MRI-PET registration with automated algorithm. J Comput Assist Tomogr 17, 536–546 (1993).



1 thought on “A Brief History of Image Registration: Part 1”
Comments are closed.